Researchers Find Muscle Stem Cells With Potential Clinical Applications
Researchers at the University of California published a study entitled “Human Satellite Cell Transplantation and Regeneration from Diverse Skeletal Muscles” in the journal Stem Cell Reports whereby they reveal isolated human muscle stem cells capable of repairing damaged muscles.
One of the major problems of treating patients with muscle injury and paralysis of small muscles of the face, hand and eye is the loss of muscle stem cells. Although surgeons are able to restore damaged nerves, the surrounded injured muscles fail to recover. “This is partly why we haven’t had major progress in treating these patients in 30 years,” said Jason Pomerantz who led the research team in a news release. “We know we can get the axons there, but we need the stem cells for there to be recovery,” he explained.
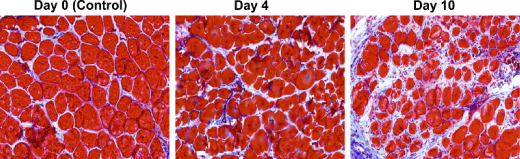
Researchers identified surface markers, known as CD56 and CD29, on muscle stem cells obtained from surgical biopsies of human trunk, limbs, and head muscles. Using this molecular signature, the research team was able to isolate cells at the borders of muscle fibers, so-called “satellite cells” found at a frequency of 2–4 cells/mm of fiber. They then grafted these cells into mice with damaged muscles induced by a toxin who were irradiated to deplete their own muscle stem-cell populations. Within five weeks, the human cells reconstituted the stem cell niche repairing damaged mouse muscle tissue.
Isolation of human muscle stem cells and their transplantation will have major implications in the therapy for paralysis patients whose damaged muscles have lost their regenerative capacity. “This gives us hope that we will be able to extract healthy stem cells from other muscles in the patient’s body and transplant them at the site of injury,” Pomerantz said. “If replenishing a healthy muscle stem cell pool facilitates reinnervation and recovery, it would be a significant leap forward.”
Importantly, the research team will continue to investigate these muscle stem cells for further understanding of muscle regenerative capacity during normal aging or in genetic diseases such as muscular dystrophy.
Read More Recent News






