White Matter Brain Lesions May Be Linked to Cognitive Dysfunction in Myotonic Dystrophy Type 1
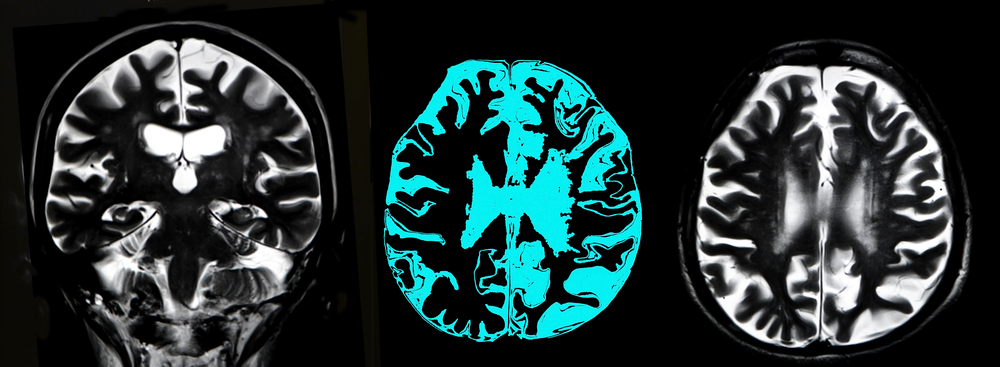
A retrospective analysis of the brain structure by MRI shows alterations in white matter in patients with myotonic dystrophy type 1 (DM1) disease. These findings suggest the brain is involved in DM1 in addition to the muscular and systemic symptoms already affecting these patients.
The study, “MRI findings and cognitive functions in a small cohort of myotonic dystrophy type 1: Retrospective analyses,” was published in the Neuroradiology Journal.
DM1 is a progressive disease that affects several systems in the body and is caused by a genetic defect. The disease is characterized by muscular and systemic symptoms, including daytime sleepiness, fatigue, defects in visual perception of the spatial relationships of objects, and anxiety.
Previous reports have suggested the brain may be involved in DM1. But how much the central nervous system (CNS) is part of the disease is not entirely clear. Some studies have reported impaired mental function associated with nonspecific disease findings, such as white-matter hyperintense lesions (WMHLs, which reflect changes in the cerebral white matter), ventricular enlargement, and brain atrophy on brain MRIs in DM1 patients.
But while some studies associated alterations in the brain with neuropsychological and clinical features of the disease, others have not found the same evidence.
Here, authors performed a retrospective analysis of brain abnormalities, looking particularly at WMHLs, and how they correlate with clinical and cognitive deficits in a small, well-characterized cohort of DM1 patients. They investigated brain alterations by analyzing patients’ cranial MRI data.
The 13 analyzed DM1 patients generally showed a moderate muscular impairment and impaired cognitive performance in several functions, including frontal, visuospatial, naming and memory abilities, and white-mass abnormalities. The cognitive impairment is highly variable among DM1 patients, and significant cognitive impairment is observed only in some patients.
They detected WMHLs mainly in the anterior temporal, frontal, parieto-occipital and periventricular regions of the brain in these DM1 patients. Despite the low number of patients, authors observed selective progressive frontal lobe function involvement.
They also found that severe cognitive deficits occurred more frequently in DM1 patients, showing white matter damage. In fact, WMHL burden was associated with impairments in memory, executive, reasoning, and visuospatial parameters.
These results suggest that DM1 is characterized by brain involvement, and that damages to the brain’s white matter are potentially responsible for the cognitive affecting these patients.






